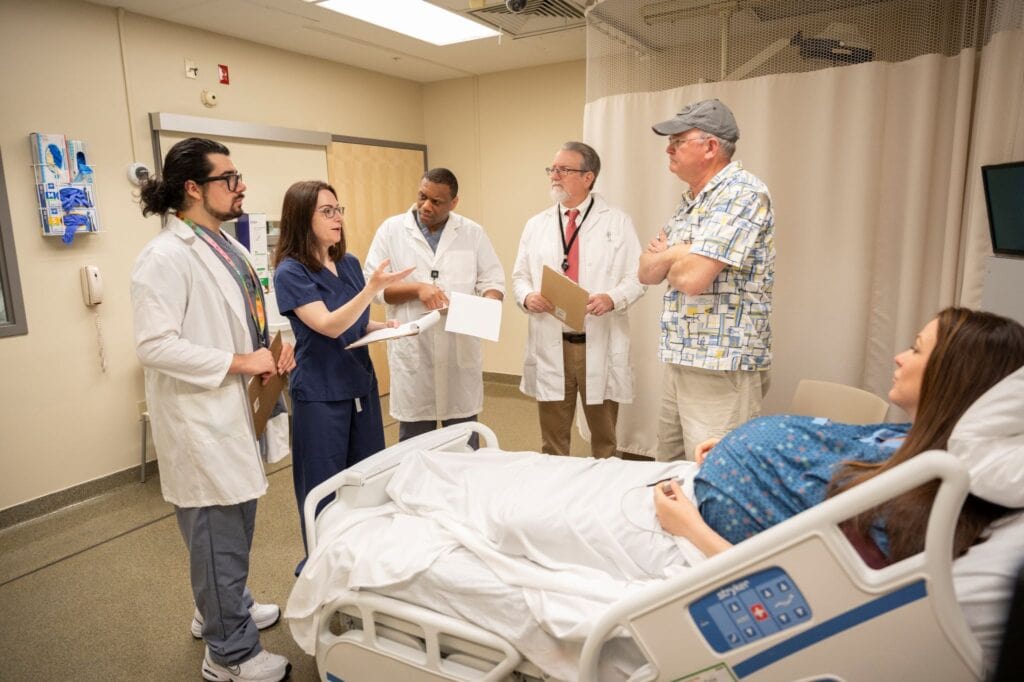
In a project involving three rural CTSA institutions, UAMS’ Karen Dickinson, M.D., is co-leading a novel effort using simulated scenarios to help health care teams manage disruptive patient encounters with providers.
Dickinson, a surgeon and interprofessional simulation education expert, is working with co-principal investigators Michael Andreae, M.D., Ph.D., professor of anesthesiology at the University of Utah, and Anita Fernander, Ph.D., executive diversity officer and professor at the University of New Mexico.
Their work was funded in 2023 by a one-year Consortium of Rural States (CORES) pilot, with each institution receiving $25,000.
“Nothing like this collaborative project has been done before in this area,” said Dickinson, director of Interprofessional Education Simulation and Clinical Skills Training at UAMS. “It’s challenging to provide this education because these are sensitive issues, but it’s important and ultimately benefits both providers and patients.”
The simulated scenarios, based on real-life experiences, feature patient behaviors that create difficult communication challenges for providers. The incidents have been created as part of a multi-step process in which a comprehensive simulation-based educational program is being created to equip health care teams with the tools to manage such situations.
In addition to helping clinical teams manage challenging patient interactions, the project addresses how these situations create a barrier to translational science, negatively impacting the stability of the clinical research workforce.
The CORES pilot is providing the resources to develop and record simulated scenarios. Health care providers who have experienced these challenges will watch the videos, and experts in cognitive task analysis will follow up with structured interviews to gain participants’ perspectives and glean details from their personal experiences. The results will inform development of a simulation-based education program.
“This work is needed because it’s a common experience, and it can be very detrimental on multiple levels, most importantly to the patient-provider relationship,” Dickinson said. “We chose simulation as an active learning strategy to support and equip all members of the team to deal with this situation.”
The collaboration was inspired by the 2022 American College of Education Accredited Educational Institute (ACSAEI) initiative to collaborate with the ASA Simulation Education Network (SEN) at the annual Surgical Simulation Summit meetings to foster interprofessional simulation education. The meeting generated connections between UAMS and the University of Utah, which led to the collaboration with the University of New Mexico.
“Conversations were already happening as a result of the ACSAEI and ASA SEN meetings, then we learned about the CORES pilot opportunity, and we knew it could really help get this project off the ground,” Dickinson said.
Other UAMS co-investigators on the project are Faiza Khan, M.D., an associate professor, and Rania Elkhateb, M.D., an instructor, both in the Department of Anesthesiology.
She is excited to be working with experts in other fields and seeing how the multi-institutional effort benefits the project.
“We’re all bringing complementary knowledge so that we can do together what we could never do individually,” she said. “Without the CORES grant, there’s no way we could have done this as effectively as we are.”